Any good rom-com starts with a “meet cute.” You know, the scene where the two main characters bump into each other on the street, spill a coffee, lock eyes, and suddenly everything changes. 😍
No one’s slow-motion-running through an airport in this example, but New Vista—a community behavioral health center and CCBHC in Kentucky—had a similar kismet moment in their technology journey.
When they paired an open-access intake model with artificial intelligence (AI), sparks flew (figuratively, of course). And more importantly, the pairing helped them expand access to care while protecting clinician time and attention.
Nikki Stanaitis, MSW, LCSM, Chief Clinical Officer of New Vista, sat down with Dr. Denny Morrison on the No Notes podcast to share what it looked like to:
- Redesign intake for faster access to care,
- Support staff through major workflow changes, and
- Improve client engagement and clinician presence.
Listen to the full episode here, or keep reading for the Hallmark moments.
The Back Story
New Vista didn’t wake up one day and decide to overhaul intake for fun.
The catalyst was becoming a Certified Behavioral Health Clinic (CCBHC)—a shift that raised the bar on timely access and forced a hard look at whether their existing systems were built to sustain it.
“We knew, in becoming a CCBHC, the importance of getting people into care quicker,” said Stanaitis. “As soon as they want care, we wanted to get them into care—but the reality was that our system was not built that way.”
Like many organizations, New Vista aimed for a same-day, next-day model. But as the schedule filled up, the intakes got “pushed out and out and out.”
When appointments get pushed out, engagement suffers—and that showed up in New Vista’s no-show rates prior to the shift with:
- 30% no-show rates for initial appointments, and
- 42% no-show rates for second appointments.
To truly meet the spirit of CCBHC access standards, they needed to shake things up. So, they moved to an open-access model, setting daily intake hours where people could walk in and be seen.
For clients, that meant faster access to care. For clinicians, it meant:
- More intakes,
- Less predictable schedules and workflows,
- Higher acuity, and
- Heavier documentation demands.
Unfortunately, opening the front door wider inevitably increases the pressure behind it.
That’s where AI entered the storyline.
The “Meet-Cute”
To keep up with an open door, something had to give behind the door.
“Becoming a CCBHC means you look at your system in new ways,” Stanaitis explained. “So when we looked at our system, we were really interested in: What are the things that we can do to help improve the overall quality of what we’re doing and the quality of services we’re providing?”
Those questions led them to explore AI—not to push clinicians to do even more with less, but to give them meaningful support in the work they were already doing.
The ability to be more present in sessions and less consumed by documentation was exactly what their clinicians needed to support the added pressure of an open-access model.
“It just fit really naturally together,” Stanaitis said.
Open access changed the client experience. AI changed the clinician experience. And together, the shift was a whole lot smoother for everyone involved.
The Perfect Match
Knowing that AI was the answer didn’t mean they rushed into adoption. New Vista leadership evaluated multiple AI documentation platforms, aware that the market was crowded and rapidly changing.
“There are a lot of options out there,” Stanaitis shared. “Often it’s part of a much larger array of services—this one little thing among many.”
That wasn’t what they were looking for.
In a space changing as quickly as AI, New Vista wanted more than a feature in a broader product suite. They wanted a company whose “jam” was clinical documentation innovation—one that was continuously refining its platform based on real-world clinical feedback.
As they spoke with peers and reviewed how different platforms had evolved over time, it became clear that some tools were built for the moment.
Instead of a static tool solving today’s problems, they were looking for a strategic partner that would anticipate tomorrow’s.
“Eleos keeps staying on the cutting edge,” said Stanaitis. “To be part of that and see how it can do more and more, and in better ways, be more nimble and user-friendly is critical.”
In rom-com terms, Eleos wasn’t just a casual date, but a relationship built to last.
For a deep dive into evaluating AI solutions for your organization, check out our Advanced Buyer’s Guide for Behavioral Health.
When It’s Not Love At First Sight: Navigating AI Skepticism
Even with all the movie magic, love stories never jump straight to the happy ending.
While Eleos felt like the right strategic fit for the organization, it wasn’t immediately admired by everyone on staff.
Like the classic “will-they-won’t-they” trope, there was healthy skepticism at first. Some clinicians were already experimenting with AI tools—though not always in ways leadership felt were secure or sustainable. Others questioned whether AI belonged in the sensitive therapeutic relationship at all.
“We had staff using AI in different ways,” Stanaitis shared. “And we as an organization really had to start deciding: What are our stances? What can you use? Because it’s being used. And if you do nothing, then it’s the Wild West out there.”
For those team members already using AI, formal adoption felt like clarity. It meant having an approved, supported solution—not a secret “side quest.”
So, they welcomed Eleos. But others were a bit more cautious.
Some clinicians worried about bringing AI into sessions. How would it affect client privacy and trust? Others were concerned about documentation remaining a core clinical skill. If AI helps write the note, do I lose some of my expertise?
Ultimately, what made the difference was the support New Vista provided in partnership with the Eleos training squad. They hosted town halls and shared information about the new platform transparently. They surfaced concerns openly and paired folks who were a bit more skeptical with Eleos representatives to have open conversations about their concerns.
As Stanaitis put it, “Nothing we were experiencing was novel. [Eleos] has been through all these different spaces where staff have said all these same things.”
Once clinicians completed training and saw how Eleos worked, hesitation shifted to curiosity. And by the end of that onboarding and implementation, curiosity shifted to excitement about all the ways AI could help them.
In fact, the shift was so dramatic that one clinician told Stanaitis, “I love Eleos so much that if I had another child, I’d name it Eleos.” She replied, “If you’re willing to name your child, that’s when you know it’s real.”
So no, it wasn’t love at first sight for New Vista staff. It was more of a slow burn—with confidence building as clinicians experienced firsthand how AI could support, rather than replace, their clinical judgment.
The Turning Point: Results That Changed the Plot
Then, there’s the moment when everything starts to fall into place. For New Vista, that moment didn’t arrive with dramatic music. It arrived in the data.
As open access and AI settled into daily operations, early indicators began to tell a clear story—not just about efficiency but about experience.
What Changed for Clients
The initial impact showed up where New Vista set out to make a change in the first place: In client access and engagement.
They saw:
- A 5% increase in daily intakes,
- Reduced time to first appointment, and
- A 16% increase in engagement/length of stay.
The first two metrics reflect the improved access that came from their new intake model, while the rise in client engagement is directly tied to what was happening in the session.
“The initial feedback that kind of went with the qualitative components that we were hearing from clinicians and from support staff is that they were able to be more present,” Stanaitis shared.
When clinicians aren’t splitting their attention between the conversation and their keyboard, the interaction changes. The therapeutic connection strengthens. And that early connection in the first few appointments often determines whether someone comes back.
Presence, it turns out, is an engagement strategy.
What Changed for Clinicians
On top of the benefits for clients, that shift in presence translated into major improvements for clinicians.
In an internal review of clinicians who worked both before and after implementation, New Vista found that within the first five months, there was a:
- 12% increase in unique clients served,
- 25% increase in services delivered, and
- 15% increase in productivity hours.
While those numbers are impressive, the productivity and caseload growth weren’t actually the goal.
“We want to give better care,” Stanaitis emphasized. “We want to give our staff everything that they need to be able to be successful.”
The productivity gains were a byproduct of reducing the documentation burden. Because when clinicians save time on notes, they gain something more valuable than margin. They gain bandwidth to see another client, to decompress, and to stay in the field they set out to make a difference in.
The Workforce Plot Twist
While it’s still early to measure the long-term impact on retention, New Vista is already seeing anecdotal signals in hiring and workforce stability.
“One of the key factors is having something like Eleos,” Stanaitis shared. “When you do have more on your plate, it doesn’t feel as hard, and it’s something to offer people right out the gate to be like, ‘this is a support tool—we want to help.’”
In a competitive hiring environment, that matters. But beyond recruitment, clinicians themselves reported a tangible shift in their day-to-day experience.
One clinician shared: “With Eleos, I’m more present during sessions. I no longer have to worry about jotting down notes. I’m able to put my laptop aside and completely focus on the client.”
That kind of feedback points to something operational leaders know well: When work feels more manageable, people are more likely to stay.
The Box Office Numbers: Organizational ROI
Every good love story eventually faces the practical questions.
Is this sustainable?
Is this working long-term?
Are we really in this together?
Within the first three to four months of implementation, New Vista started looking at the numbers—not just the feelings. Call it “defining the relationship.” 😉
Leadership evaluated the organizational impact of Eleos through productivity gains and reclaimed documentation time, asking a straightforward question: Is this delivering real value?
Early Pay-Offs
The answer came quickly. Initial findings in the first five months showed that the platform was on track to pay for itself. (Yup, you read that right.)
“Overall, we were able to determine that we are on the trajectory financially to pay for the product itself based on the savings,” said Stanaitis.
Here’s what that looked like:
- 35,000+ notes completed using Eleos,
- 4,600 hours saved (so far), and
- At least three hours saved per clinician per week.
For clinicians completing an average of 77 notes per week, that time savings adds up fast.
And since recording the podcast, these gains have continued to grow. New Vista has seen a $173K increase in billable services.
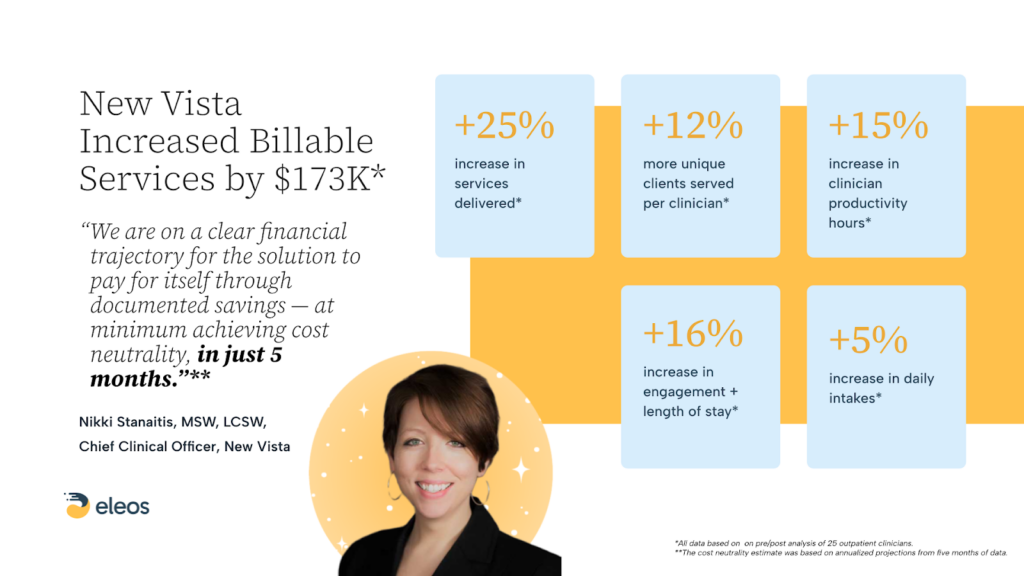
With numbers like that within months of rollout, you could call the implementation a success. But for New Vista, that was only “Act One.”
Turnover Savings
On top of time savings, Stanaitis was clear on another metric New Vista was paying close attention to: Turnover.
“Every time a staff member leaves, we know that there’s a cost to recruitment, but there’s also a cost to the clients being served,” Stanaitis explained.
When a clinician leaves:
- Caseloads have to be transferred,
- New clinicians have to ramp up,
- Productivity dips during transition, and
- Clients may disengage altogether.
Retention, then, becomes more than an HR metric. It’s a continuity-of-care strategy.
That initial intake experience sets the tone. If the first session feels rushed or overly transactional, the connection may not be strong enough to withstand a client handoff later, if a clinician were to leave.
“We have clients who are transferred, they meet with their clinician and then are like, ‘This is not the person I had met,’” Stanaitis shared.
But when clinicians are more present—when the conversation feels organic rather than clunky—the foundation is stronger from the start.
“If you’re able to sit down in that first session and have a real conversation and it feels organic,” Stanaitis explained, “you might transition and retain somebody better.”
In other words, having that AI documentation support doesn’t just reduce burden. It strengthens clinicians’ presence, so their first impressions with clients are stronger—making transitions smoother later… if they have to happen at all.
Beyond the Early Returns
As New Vista continues to evaluate long-term impact, leadership plans to look beyond direct productivity savings to measure:
- Reduced recruitment and onboarding costs,
- Improved staff retention,
- Stabilized caseload transitions, and
- Sustained client engagement.
“There are several layers of organizational-level power that come from using this tool—and using it well,” Stanaitis added.
Because the real organizational payoff isn’t just in hours saved. It’s in creating an environment where both clinicians and clients want to stick around.
This story isn’t a one-off. Check out how Gulf Coast Center gained 8x ROI with Eleos.
The Closing Scene: Lean Into Change
For leaders navigating rising demand, workforce strain, and policy uncertainty—including the ripple effects of H.R.1 Medicaid cuts—Stanaitis’ advice was clear:
“If you’re ready for a deep change, I encourage you to lean into it.”
There were moments when New Vista could have taken the easier path. Moments when it would have been simpler to continue business as usual. Instead, they dedicated a team, re-evaluated workflows, and committed to doing the work.
“Business as usual is dead,” Stanaitis emphasized. “You really do need to think about: How can you be better? How can you strengthen what you’re doing and do it in a way that’s sustainable?”
For her organization, that meant rethinking access, intake, and how clinicians were supported in their day-to-day work.
In the end, open access allowed New Vista to expand care to more clients, and AI restored the time and documentation burden that came with it. And that’s where Stanaitis’ advice becomes even more direct. When it comes to AI, she urged leaders not to ignore it.
Evaluate thoughtfully. Decide intentionally. But don’t let hesitation determine where your organization will be five years from now.
For New Vista, the “meet cute” wasn’t just a clever analogy. It was a strategic shift—one that improved access, supported clinicians, and positioned the organization for sustainable growth.
Because the right match doesn’t just create sparks. It creates staying power.
If your reaction to New Vista’s results is something like, “We’ll have what they’re having,” it may be time to explore what that looks like in your own organization.
Request a personalized demo today to see how Eleos can support sustainable access and clinician capacity.

