Revenue Cycle Management
Maximize revenue integrity before claim submission
Prevent eligibility errors and coding gaps that cause denials, write-offs, and rework—acting at the point of care, before problems compound. Your billing team handles exceptions. Eleos handles everything else.
Sustainable Revenue Health
Ensure your organization realizes the full value of the care provided. By gently catching coding and duration errors early, you reduce the need for write-offs and protect your long-term stability.
Predictable Reimbursements
Move away from the uncertainty of “rejection-and-resubmit” cycles. Higher first-pass acceptance means a steadier, more dependable flow of resources back into your programs.
Targeted Operational Focus
Help your RCM staff breathe easier. By focusing only on the exceptions that truly need their expertise, you reduce manual fatigue and allow your team to work more effectively.
In community-based care, the most expensive billing errors happen before a claim is ever submitted.
Most organizations don’t have a collections problem. They have a prevention problem. Eligibility errors, inactive coverage, and payer switches don’t get caught until after services are delivered—and by then, the rework is expensive and the cash flow already delayed.
Without Eleos
Eligibility gaps surface after services are delivered—denials, write-offs, rebilling.
With Eleos
Eligibility is verified before services are delivered. Your team handles exceptions. Not everything.
Revenue protected at every step—from point of care to claim.
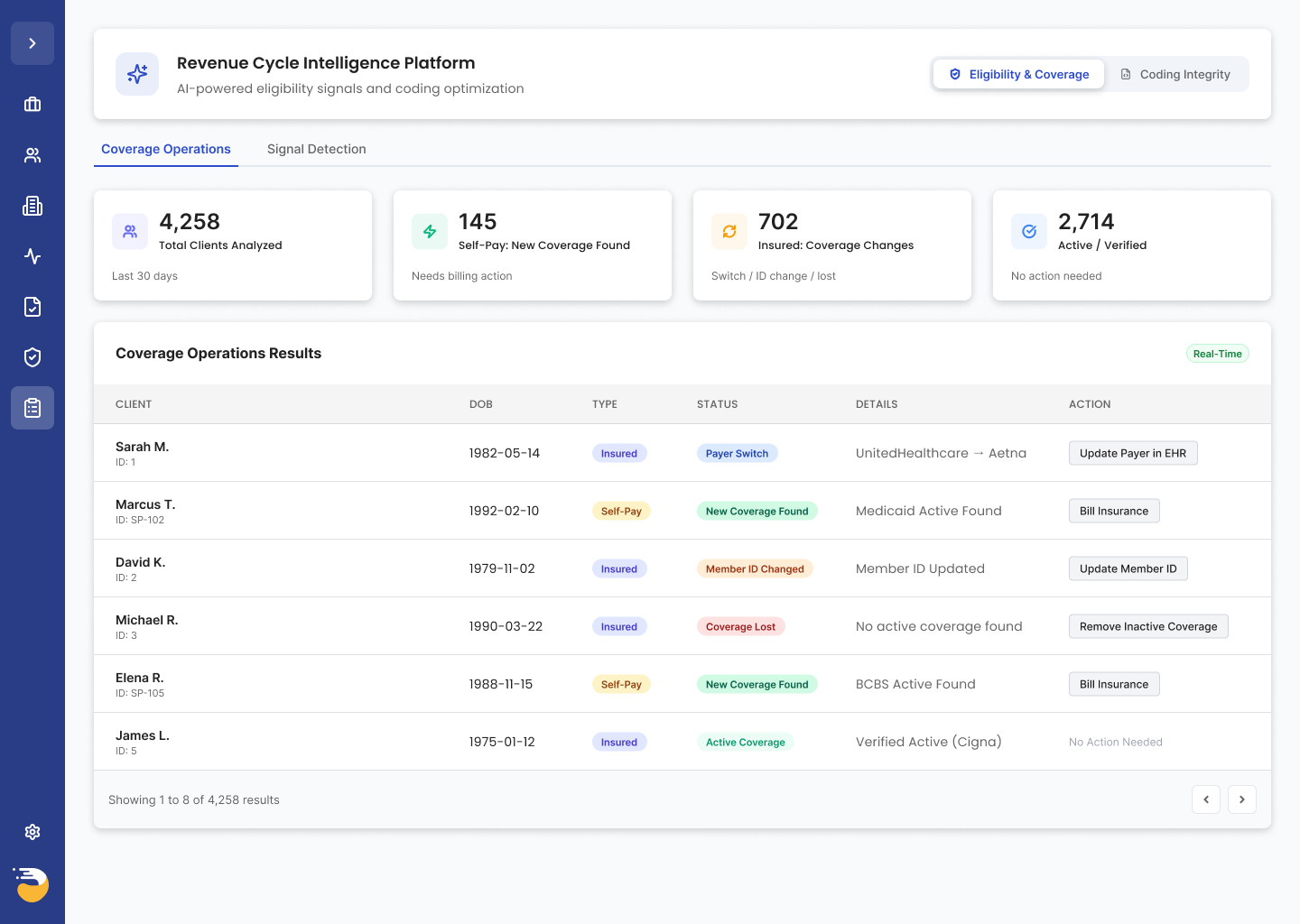
Eligibility Intelligence
Full visibility before the claim goes out.
Eleos gives your billing team everything they need to submit clean claims—hidden coverage found, payer switches caught, coverage lapses flagged—before services are delivered. Early partners have seen 8.5× ROI on eligibility alone, a 25% reduction in uninsured clients, and hundreds of thousands of dollars recovered. Every finding comes back as a per-patient action row, already triaged. Your team doesn’t have to interpret anything. They just act.
Payer switches, coverage lapses, and hidden coverage surface before the appointment—so nothing goes out the door incomplete.
Without Eleos
A patient’s plan changed and no one caught it — the claim gets denied three months later. A self-pay patient was covered the whole time and no one knew.
With Eleos
Payer switches, coverage lapses, and hidden coverage surface before the appointment—so nothing goes out the door incomplete.
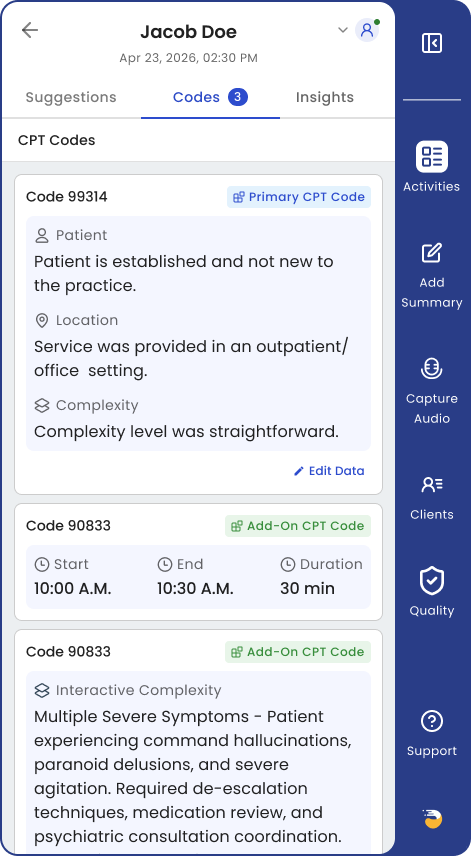
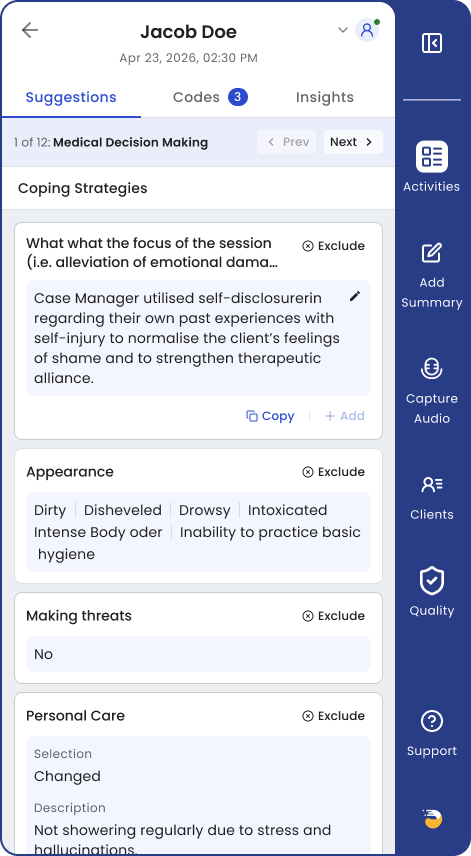
Coding Optimization
Bill what you’ve earned.
Revenue slips through at the point of documentation—incorrect code selections, session time not fully captured, procedure codes that don’t get applied. Small gaps at this stage can quietly add up.
Because Eleos is already present in the session, it can surface relevant information at the point of documentation—helping ensure session time is accurately captured and that the right codes are applied based on what took place. It’s a suggestion, and the provider always decides. Control stays in human hands.
Without Eleos
A lower E/M code gets selected to stay safe. A 53-minute session gets logged as 50. The gap is invisible—until you add it up across a month.
With Eleos
The right code is surfaced at the moment of documentation, with the session content to support it.
“Eleos is a game changer in eligibility automation, we saw a 8.5x ROI on our investment.”
 Sarah Stockwell
Sarah Stockwell
Chief Financial Officer, CrossWinds
Purpose-built for community-based care organizations where every dollar of recovered revenue matters.
Built for community mental health centers, CCBHCs, substance use disorder treatment organizations, and care at home providers—the settings where reimbursement pressure and staffing costs leave the least room for preventable revenue loss.
Prevention, not cleanup.
The denials that cost you the most are the ones that were preventable. Eleos acts before claims go out the door — so your team never has to chase them.